What is nest?
- A simple blood test determining the future health of your baby
- Safe from procedural risks of invasive procedures (chorionic villus sampling (CVS) & amniocentesis)
- Lowest test failure rate with inclusion of fetal fraction
- Fast results – usually available to your doctor within 5 business days
nest is a simple blood test that screens for the most common chromosomal conditions that can affect your baby’s health. nest offers parents-to-be a new choice to obtain important information about the health of their developing baby, simply, accurately and in the first trimester (at 10 weeks), with little or no risk to their pregnancy. It is performed in Australia and is the only test of its kind that is supported by Genetic Counselling
A blood sample can be drawn at any of our collection centres as early as the 10th week of pregnancy.
nest is available for both singleton and twin pregnancies.* Test results are usually reported back to your healthcare provider within 5 business days.
* Sex chromosome aneuploidy testing is available for singleton pregnancies only.
Click here to view our collection centres.
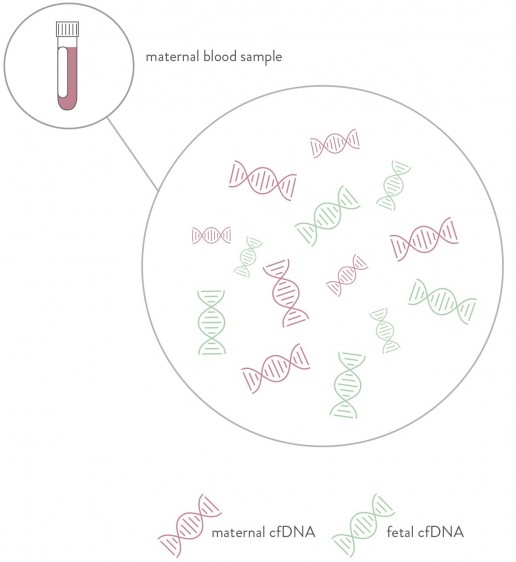
A sample of your blood is drawn and the genetic material (DNA) from you and your baby is tested. The nest screening takes a deeper approach to the science, using an advanced technology called ‘Massively Parallel Sequencing’ to analyse millions of DNA fragments per sample and accurately count the number of chromosomes present. It then uses a special SAFeR™ calculation method to determine if your baby has too many or too few copies of these chromosomes.
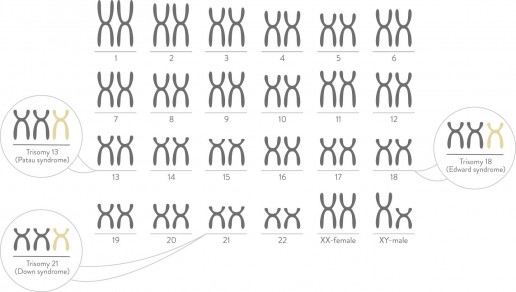
Chromosomes normally come in pairs. Most individuals usually have 23 pairs of chromosomes. nest looks for too few or too many copies of chromosomes. Missing or extra copies of chromosomes can be associated with intellectual or physical disabilities, with different levels of severity. The most commonly seen chromosomal conditions listed below can be accurately detected with nest.
Trisomy 21 Down syndrome
Carrying an extra copy of chromosome 21 causes Down syndrome. People born with Down syndrome can have health and development challenges, some level of intellectual disability and have some characteristic physical features.
Down Syndrome is the most common chromosome disorder affecting approximately one in every 660 pregnancies in Australia.
Trisomy 18 Edwards syndrome
Carrying an extra copy of chromosome 18 causes Edwards syndrome.
High rate of miscarriage is often associated with Edwards syndrome. Additional babies born with the condition have a significantly shortened life expectancy, suffer heart abnormalities, kidney malformations and developmental delays.
This is the second most common chromosome disorder affecting approximately one in every 1,100 pregnancies in Australia.
Trisomy 13 Patau syndrome
Carrying an extra copy of chromosome 13 causes Patau syndrome.
Again, with trisomy 13 high rate of miscarriage is often associated. Babies born with Patau syndrome rarely survive beyond the first year of life. They often suffer eye defects and difficulties with feeding and breathing, heart and brain problems.
Approximately one in 3,000 pregnancies in Australia are affected by Patau syndrome.
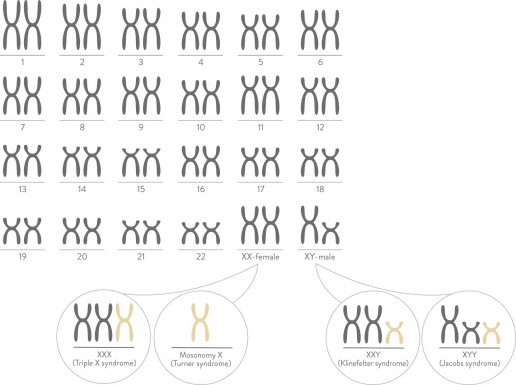
Gender Screening
nest is also able to detect gender. Men normally have an XY pair of sex chromosomes. Women normally have an XX pair of sex chromosomes. If your doctor chooses, nest can also be used to screen for sex chromosome conditions You can elect to have gender disclosed to you or not.
- Turner syndrome – only one X chromosome in a female
- Klinefelter syndrome – an extra X chromosome in a male
- Triple X
- Jacobs syndrome- an extra Y chromosome in a male
Today there are a number of genetic testing options available for expectant women and doctors. Some tests are called ‘screening’ tests and others are called ‘diagnostic’ tests.
Traditional screening tests are used to predict the chance of a pregnancy having certain chromosomal conditions. Results from screening tests usually provide a ‘risk score’ (such as 1 in 500 or 1 in 50) that describes the chance of a baby having a certain chromosome conditions. They do not provide definitive answers and can have a relatively high rate of ‘false negative’ or ‘false positive’ results. But not all screening tests are the same in terms of accuracy and convenience.
Diagnostic tests, such as amniocentesis or chorionic villus sampling (CVS), can accurately determine whether a pregnancy has trisomy 21 (Down syndrome) or other chromosomal conditions. However, these procedures are invasive and carry a risk of miscarriage.
The nest screening test sheds much needed light on the chromosomal health of your unborn baby providing the reassurance of reliable answers no other screening test can match. Compared to similar options, nest offers a highly precise chromosome screening, rather than calculating chances or risk scores. And, it does not carry the risk of miscarriage that an invasive procedure can.
Your results will tell your doctor whether or not trisomies 21, 18, 13 or sex chromosome conditions (if ordered) are highly likely to be present in your pregnancy. In the case of a high probability result, your doctor and Genetic Counsellor will discuss what the results mean to your pregnancy as well as further testing options to consider.
Your test report will include one of two possible results for chromosomes 21, 18, and 13:
- Low Probability—means the expected number of chromosomes was found.
- High Probability —means too many or too few copies of one of the chromosomes have been identified.
This can indicate a chromosome condition. Diagnostic testing is recommended for confirmation.
If the sex chromosome option is ordered, results will be reported as either Low Probability or High Probability. If gender is requested this will be labelled male or female.
Highly trained nest Genetic Counsellors are available if requested by your doctor to explain the technology and how the results will be reported. They can also deliver your results. Having a deep understanding of this technology gives them the skills to interpret these results and assist in explaining them. If the results do come back showing a high probability result, the skills of the Genetic Counsellor can assist in explaining the next steps.
nest is a highly accurate advanced screening test that is non-invasive. No test, however, can guarantee a baby will not have any medical issues. nest only looks at chromosomes 21, 18, 13, and sex chromosomes*, if ordered. It does not test for or report all genetic and nongenetic problems that may be present in a baby. If the test result is Low Probability result, it does not completely rule out all potential problems associated with chromosomes 21, 18, and 13, or all sex chromosome conditions in your baby.
Genetic counselling can be made available to all patients by their requesting doctor to assist in understanding what to expect from the results. Women who receive High Probability results should be offered invasive prenatal procedures for confirmation.
A Low Probability result does not ensure an unaffected pregnancy. CVS and amniocentesis provide definitive diagnostic information, but the invasive nature of these procedures means that they are generally only offered to those who have been identified as a high-risk pregnancy.
* Sex chromosome aneuploidy testing is available for singleton pregnancies only.
The performance of nest was evaluated in a major scientific study in which more than 60 leading US medical research and teaching institutions participated. The study findings were reviewed and published in the leading journal read by obstetricians and gynaecologists. A second study, published subsequently, presented the test’s performance under regular clinical conditions and found similar results.
References
- Bhatt S, Parsa S, Snyder H, Taneja P, Halks-Miller M, Seltzer W, DeFeo E. Clinical Laboratory Experience with Noninvasive Prenatal Testing: Update on Clinically Relevant Metrics. ISPD 2014 poster.
- Bianchi DW, Platt LD, Goldberg JD, et al. Genome-wide fetal aneuploidy detection by maternal plasma DNA sequencing. Obstet Gynecol. 2012;119:890–901.
- Futch T, Spinosa J, Bhatt S, de Feo E, Rava RP, Sehnert AJ. Initial clinical laboratory experience in noninvasive prenatal testing for fetal aneuploidy from maternal plasma DNA samples. Prenat Diagn. 2013;33:569-574.